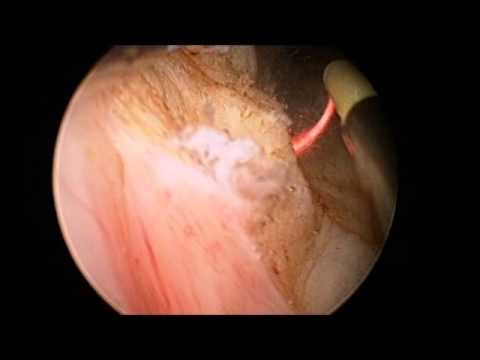
Transurethral Resection of the Prostate (TURP)
TURP involves an instrument being inserted up the urethra in order to remove a section of the prostate that is blocking the patient’s urine flow. Urologists often recommend TURP if symptoms of enlarged prostate (BPH) do not respond to home treatment or meds. TURP is now the most common surgery Urologists employ to remove part of an enlarged prostate.
Types of TURP
- Monopolar TURP: Conventional TURP removes tissue with a wire loop that has electrical current flowing in one direction (monopolar) through the resectoscope to cut the tissue. The surgical site is irrigated with nonconducting fluid. The fluid prevents the electrical current from disturbing surrounding tissues, but it can damage surrounding tissue after prolonged exposure, resulting in TUR syndrome. This limits surgery time.
- Bipolar TURP: A newer technique, Bipolar TURP uses bipolar current to remove the tissue. Because it allows for saline irrigation (instead of nonconducting glycine as in monopolar TURP) it reduces complications such as TUR syndrome. This allows for longer procedure length.
- Plasmakinetic resection: PK or Button resection uses ionized vapor that heats up by low voltage electricity a semi-spherical button to vaporize the prostate tissue from inside. This is considered to be the least intrusive of all current techniques. It also features fewer post-op complications and shorter healing time.
After the TURP Procedure
The patient will typically be hospitalized for one to two days. The patient will be catheterized to remove potential blood and blood clots from the bladder. When the urine is relatively clear of blood, the patient is typically discharged. The patient should avoid strenuous activity and sexual activity for about six weeks. Also during that time, the patient should avoid fecal constipation that would cause strain in the bathroom. Laxatives may be required.